Our Local Hospital is Prepared
Dec 2, 2020

Miller Report for the Week of November 30th, 2020
By William Miller, MD – Chief of Staff at Adventist Health – Mendocino Coast Hospital
Since the beginning of this pandemic, we expected that the summer months would bring a slowing in the spread of the virus with a significant increase during the winter months. That is what we are seeing now. Preparing for this predicted scenario is what Adventist Health Mendocino Coast (AHMC) and most other hospitals across the country have been doing since March. When we read scary news reports that ICU’s in California may reach 112% of capacity by Christmas, temper this with the understanding that oursurge capacityplanninghas specifically been about getting ready to deal with cases exceeding normal capacity. This planning was mandated in March by the California Department of Public Health of all hospitals in the state. While this pandemic has been fraught with many challenges, such as inadequate community surveillance testing which continues to be a frustration, there has been good coordination between hospitals, county health departments and the state health department.
A big boost to our local planning and preparedness came when we affiliated with Adventist Health (AH). To be sure, some hospitals within the AH system are experiencing significant COVID caseloads that have pushed them well into their surge plans. This is especially true for those in the southern part of the state. However, at the same time, belonging to a system allows for resources to be directed towards those areas most in need. Thus, those facilities currently being hit hardest are getting the support that they need from AH. If needed, we expect to receive the same support out here on the Coast.
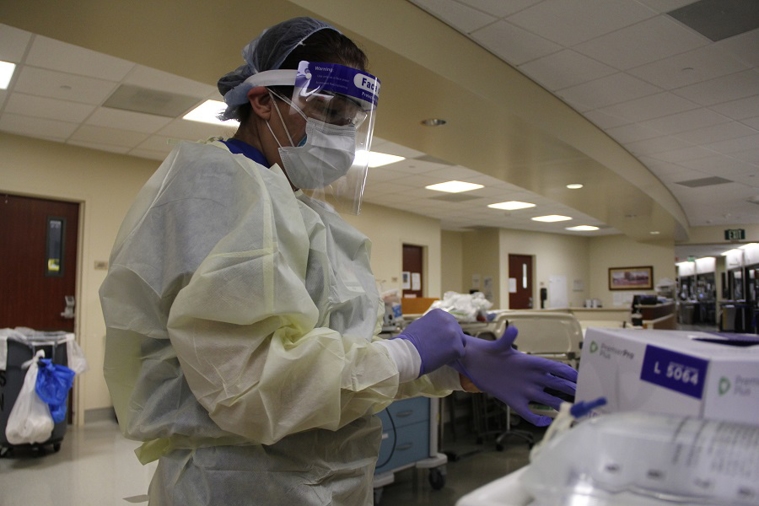
Here in Mendocino County, we have already benefited by having all three of our hospitals working together on one combined strategy. A coordinated strategy is far more powerful than when we were left to plan on our own before the affiliation. Some specific benefits include adequate stocks of personal protective equipment (PPE), easier access to COVID treatment medications, assistance with getting testing reagents to test our patients, and if things get really serious for us, then access to AH staff pools and an AH emergency ventilator sharing agreement.
Our surge plan is something that we periodically review and a work group of our local hospital leaders recently updated our plan. This group included folks like Davey Beak, the head of our ambulance service, who has done an outstanding job throughout this pandemic as our local incident commander. It also included our two local nursing managers, Kelly Hendricks, RN, for in-patient services and Anita West, RN, overseeing the emergency department. Both are excellent leaders who have helped hold us together as a team from the very beginning. The group also included additional all-stars: Heather Brown-Douglas, RN, our Director of Quality; Lois Leister, Director of Pharmacy; Mary Nivens, RN, Director of Surgical Services; and Joyce Boghosian, RRT, Emergency Preparedness Manager.
Much of our surge plan has evolved as a result of our experience during the Sherwood Oaks outbreak. During that outbreak, we opened an entire 9 bed ward as a designated COVID unit. That unit stands ready to be reopened if needed. Along with our COVID unit, we have additional expansion capabilities. We learned much about what worked well and what did not work as well during that invaluable, real-life experience. I am very confident that we are ready to deal with a surge of cases that may come our way in the weeks and months that follow.
We have been fortunate that up until now we have largely avoided having a lot of cases here on the Coast. That could not have possibly remained true forever and we are now starting to see our share of cases. I expect that before this is all over, each of us will personally know at least one person who has had COVID. As we consider the implications for this, keep in mind that fully 80% of all people infected never have symptoms or only mild ones like a runny nose. Twenty percent (1 in 5) will have more significant symptoms. Still, only about a third of those, or 8% of all people infected, require hospitalization with most not needing to be admitted to an ICU. The overall mortality rate remains relatively low compared to other pandemics. COVID has about a 2% mortality rate in the US.
The recent Thanksgiving holiday is certainly expected to dramatically boost cases in the next few weeks. The good news is that travel was down compared with last year. However, over 50 million Americans still moved around the country to visit friends and family. According to the TSA, 9.4 million Americans went through airport screening checkpoints during the 5 days of Thanksgiving travel (which is only 41% of the number in 2019). According to AAA, automobile travel this holiday was only 65% of last year, but still comprised about 48 million Americans.
If local people would like to help us in planning for the surge of COVID cases in our community this winter, then please do so by staying home for the holidays and ask your friends and family not to visit you from a far. As difficult as that is to accept, it is perhaps one of the most important things we can do now to help limit the rise in cases.
Related articles
Hope through adversity: Lessons to remember as we reflect on the past year and the impact of COVID-19
March 17, 2021

Raising Healthy Kids: A Blog from Your Trusted Pediatric Nurse Practitioner
May 19, 2021

The Adventist Health Mission Trip Experience: Palpable Joy and Giving Back
February 8, 2024